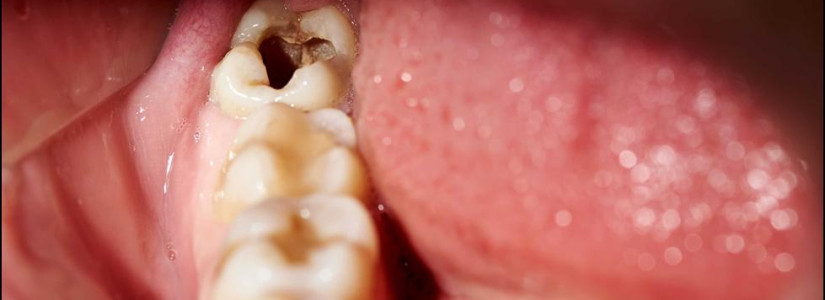
How to prevent and treat tooth decay?
Health Tips
HD Medical Team
on Tue, Feb 02 2021 12:29 PM
2970 Views
No recommendations yet !!!
Cavities are permanent and localized destruction of dental hard tissues by causing tiny openings and holes. These destructions are caused by bacteria, particularly S. mutans and Streptococcus sobrinus that are both acidogenic (acid-producing) and aciduric (able to grow at low pH). These streptococci bacteria are transmissible between humans, and infants are often infected by salivary contact with their mothers. They readily colonize the tooth surface shortly after the eruption. However, they do not become destructive and form cavities until exposed to dietary sucrose, which can be rapidly sequestered and utilized by plaque-associated organisms, including S. mutans and other acidogenic and aciduric organisms. Follow the step to prevent and treat tooth decay.
How does our body try to prevent decay?
Our oral cavity has an innate immune response that is characterized by the secretion of various antimicrobial peptides (defensins) by oral epithelial tissues in response to bacterial stimuli or inflammation. Commensal and pathogenic bacteria utilize different pathways in the production of this defensin, and epithelial cells from different body sites appear to have common signaling mechanisms to distinguish commensal from pathogenic bacteria. In addition, teeth have at least three intrinsic mechanisms that protect against carious decay. These are:
- A constant flow of saliva, which is at a neutral pH, bathes the tooth, buffers, and washes away bacterial acids, and supplies calcium and phosphate to remineralize and repair damaged tooth surfaces.
- In addition, saliva and its various constituents, such as lactoferrin, lysozyme, lactoperoxidase, beta-lysin, and immunoglobulins, possess important antimicrobial activity against plaque-associated bacteria.
- The cleansing action of the tongue and buccal membranes, which remove food particles from the proximity of the tooth.
- The acquisition by the tooth of an acellular, structureless, and bacteria-free coating are known as the acquired pellicle, which is of salivary origin and acts as a surface barrier to most dietary and bacterial acids.
What causes teeth to decay and form cavities?
There are various risk factors that can lead to decay teeth cavities. These are:
- Younger or older age: Cavities are common in very young children and teenagers. Older adults also are at higher risk. It is because, over time, teeth wear down and gums recede and makes teeth more vulnerable to root decay. In addition, older adults who use more medications that reduce saliva flow may be at more risk than others for tooth decay.
- Location of Teeth: Premolars and Molars are most frequently susceptible to dental caries and decay. As these teeth have lost pits and grooves, a lot of small food particles get collected. This results in difficulty to brush and keep teeth cleaner and smoother.
- Dry mouth: Some medical conditions, certain medications, radiation, or certain chemotherapy drugs increases the risk of cavities by reducing saliva production and causing dry mouth. Saliva helps prevent tooth decay by washing away food and plaque from the teeth and substances found in saliva also help to counter the acid produced by bacteria.
- Foods and drinks: Foods like milk, ice cream, honey, sugar, soda, dried fruit, cake, cookies, hard candy and mints, dry cereal, and chips remain in the teeth for a longer time causing decay and caries. And sipping soda or other acidic drinks throughout the day helps create a continual acid bath over teeth.
- Infant feeding habit: Feeding babies with milk, formula milk, juice, or other sugar-containing liquids during bedtime can predispose them to decay and caries. These sugar-containing food remain in their teeth for a longer time feeding decay-causing bacteria. Similar damage can occur when toddlers wander around drinking from a sippy cup filled with these beverages.
- Inadequate brushing: Inadequate brushing is another risk factor for tooth decay and carried. It is advised to clean teeth soon after eating and drinking as plaque forms quickly.
- Lack of enough fluoride: Fluoride is a naturally occurring mineral that helps prevent cavities and can even reverse the earliest stages of tooth damage. It is the most common ingredient of toothpaste and mouth rinses. Lack of enough fluoride may lead to cavities.
- Poor/Inadequate fillings or dental devices: Poor or inadequate dental fillings begin to break down and weaken over the years. This allows bacteria to build up easily and make it harder to remove. Also, ill-fitting dental fillings allow bacteria to grow underneath and yield in decaying.
- Heartburn and Acidity: Acidity and heartburn cause stomach acid to flow into one’s mouth. In addition, eating disorders like anorexia nervosa, bulimia nervosa leading to induce vomiting and causes acid to flow into the mouth. This acid erodes the enamel of teeth and causing significant damage.

What are the symptoms of tooth decay?
The signs and symptoms of cavities vary and depend on their extent and location. Common symptoms include:
- Spontaneous toothache or pain
- Sharp or mild pain when eating or drinking something sweet, hot, or cold
- Tooth sensitivity
- Visible pits, holes in the teeth
In severe cases, the pain may intervene with daily life and may lead to difficulty in eating or chewing. Other complications include:
- Tooth abscess
- Swelling or pus around a tooth
- Loss of teeth
- In rare cases, a tooth abscess — a pocket of pus that's caused by a bacterial infection — can lead to more serious or even life-threatening infections
How to treat tooth decay and dental caries?
Dental caries and cavities are commonly treated by dentists by filling them. A dentist will remove the decayed tooth tissue and then restore the tooth by filling it with a filling material.
How to prevent tooth decay and getting it worse?
The key to the prevention and control of dental caries and advanced periodontitis is the active promotion of oral hygiene. The components of such a regimen include:
- Regular brushing with a fluoridated toothpaste and dental flossing after each meal
- Dietary counseling to reduce the ingestion of sugar-rich foods or beverages
- Use of topical fluorides and oral antimicrobial rinses, such as chlorhexidine for high-risk patients
- Modification of risk factors, such as smoking cessation
- Overcoming the reluctance for regular visits to dental professionals
A variety of other measures have been effective for caries prevention. Although none of these measures is routinely applied in clinical practice, they are useful in selected patients with rampant caries.
- Xylitol gum, a nonfermentable five-carbon sugar, is a sugar substitute between meals.
- Oral antimicrobial rinses with 0.12% chlorhexidine help to control dental plaque bacteria but have no proven effect on dental caries. Although one needs to be a bit careful as Chlorhexidine has a bitter taste, stains the enamel and tongue, and prolonged application can promote the emergence of resistant microorganisms.
- Oral probiotics may be effective for caries prevention and treatment of periodontal disease in certain high-risk populations. However, more investigations are necessary to define their role in oral health and disease.


Leave a comment