Mumps is a contagious disease that is spread when infected people cough, sneeze, or talk. Sharing items, like cups or drink cans, with infected people can also spread the virus. The virus can also live on items and surfaces touched by an infected person for several hours.


MUMPS
Symptoms
Symptoms of mumps are fever, headache, muscle aches, tiredness, loss of appetite, and swollen and tender salivary glands under the ears or jaw on one or both sides of the face (parotitis). Most people with mumps recover fully. However, mumps can occasionally cause complications, such as swelling of the brain, testicles (in males), and ovaries and breasts (in females), and temporary or permanent deafness.
Causes
Mumps is caused by the mumps virus, which belongs to a family of viruses known as paramyxoviruses. These viruses are a common source of infection, particularly in children.
When you get mumps, the virus moves from your respiratory tract (your nose, mouth and throat) into your parotid glands (saliva-producing glands found either side of your face), where it begins to reproduce. This causes the glands to swell.
The virus can also enter your cerebrospinal fluid (CSF), which is the fluid that surrounds and protects your brain and spine. Once the virus has entered the CSF, it can spread to other parts of your body, such as your brain, pancreas, testicles (in boys and men) and ovaries (in girls and women).
How mumps is spread
Mumps is an airborne virus and can be spread by:
- an infected person coughing or sneezing and releasing tiny droplets of contaminated saliva, which can then be breathed in by another person
- an infected person touching their nose or mouth, then transferring the virus onto an object, such as a door handle, or work surface; if someone else touches the object shortly afterwards, they can transfer the virus into their respiratory tract
- sharing utensils, such as cups, cutlery or plates with an infected person
People with mumps are usually most infectious from a few days before their parotid glands swell until a few days afterwards. For this reason, it's advisable to avoid work or school for five days after your symptoms first develop if you're diagnosed with mumps.
Mumps can also be passed on by people who are infected with the virus but don't have any obvious symptoms.
Diagnosis
If your doctor suspects that you or your child has mumps, a virus culture or a blood test may be needed. Your immune system normally makes antibodies to help you fight an infection. So if you have mumps, the blood test can detect the antibodies in your system that are fighting the mumps virus.
Preventions
Get a mumps vaccine:
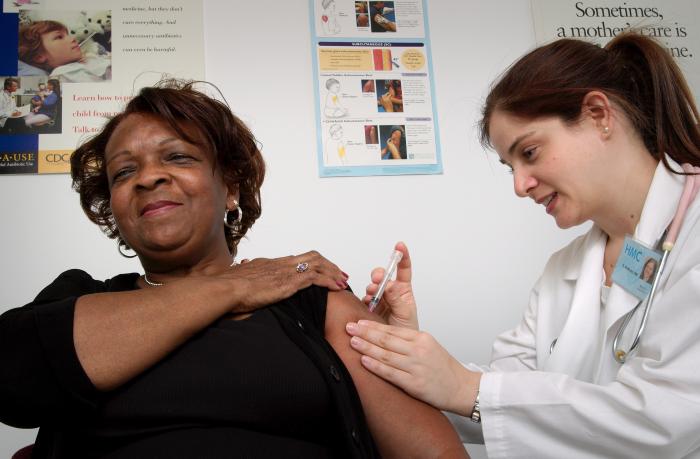
- People who cannot show that they were vaccinated as children and who have never had mumps should be vaccinated.
- The only mumps vaccines available in the United States are the measles-mumps-rubella (MMR) and the measles-mumps-rubella-varicella (MMRV) vaccines.
- Adolescents and adults who have not had mumps or have not been vaccinated with MMR should get 2 doses, separated by at least 28 days.
- Infants 6 months through 11 months of age should have 1 dose of MMR vaccine if traveling internationally.
- Children in the United States routinely receive MMR vaccination at age 12-15 months
- Children 12 months of age or older should have 2 doses, separated by at least 28 days.
- MMR has been used safely and effectively since the 1970s. A few people experience mild, temporary adverse reactions, such as joint pain, from the vaccine, but serious side effects are extremely rare. There is no link between MMR and autism.
- Two doses of this vaccine are nearly 90% effective at preventing mumps.
- See Vaccine Information Statements (VIS) for more information.
Practice hygiene and cleanliness:
- Wash your hands often.
- If soap and water aren’t available, clean hands with hand sanitizer (containing at least 60% alcohol).
- Don’t touch your eyes, nose, or mouth. If you need to touch your face, make sure your hands are clean.
- Cover your mouth and nose with a tissue or your sleeve (not your hands) when coughing or sneezing.
- Try to avoid close contact, such as kissing, hugging, or sharing eating utensils or cups, with people who are sick.
Risk Factors
Because the mumps vaccine is not used everywhere, mumps is a common disease in many countries. The risk of mumps for travelers is high in many countries of the world, including industrialized countries, such as the United Kingdom, which has had several outbreaks since 2004, and Japan, which does not routinely vaccinate against mumps. Risk is especially high for travelers older than 1 year who have not had mumps vaccine.
Complications
There are several problems that often occur with mumps. These can be worrying, but they're rarely serious and usually improve as the infection passes.
Common complications
Swollen testicle
Pain and swelling of the testicle (orchitis) affects one in four males who get mumps after puberty. The swelling is usually sudden and affects only one testicle. The testicle may also feel warm and tender.
In affected boys and men, swelling of the testicle normally begins four to eight days after the swelling of the parotid gland. Occasionally, swelling can occur up to six weeks after the swelling of the glands.
Any testicle pain can be eased using over-the-counter painkillers such as paracetamol or ibuprofen. If the pain is particularly severe, contact your GP, who may prescribe a stronger painkiller for you.
Applying cold or warm compresses to your testicle and wearing supportive underwear may also reduce any pain.
Just under half of all males who get mumps-related orchitis notice some shrinkage of their testicles and an estimated 1 in 10 men experience a drop in their sperm count (the amount of healthy sperm their body can produce). However, this is very rarely large enough to cause infertility.
Swollen ovaries
One in 20 females who get mumps after puberty experience swelling of the ovaries (oophoritis), which can cause:
- lower abdominal pain
- high temperature
- being sick
The symptoms of oophoritis usually pass once the body has fought off the underlying mumps infection.
Viral meningitis
Viral meningitis can occur if the mumps virus spreads into the outer protective layer of the brain (the meninges). It occurs in about one in seven cases of mumps.
Unlike bacterial meningitis, which is regarded as a potentially life-threatening medical emergency, viral meningitis causes milder, flu-like symptoms, and the risk of serious complications is low.
Sensitivity to light, neck stiffness and headaches are common symptoms of viral meningitis. These usually pass within 14 days.
Pancreatitis
About 1 in 20 cases of mumps lead to short-term inflammation of the pancreas (acute pancreatitis). The most common symptom is sudden pain in the centre of your belly. Other symptoms of acute pancreatitis can include:
- feeling or being sick
- diarrhoea
- loss of appetite
- high temperature
- tenderness of the belly
- less commonly, yellowing of the skin and the whites of the eyes (jaundice)
Although pancreatitis associated with mumps is usually mild, you may be admitted to hospital so your body functions can be supported until your pancreas recovers.
Rare complications of mumps
Rare but potentially serious complications of mumps include an infection of the brain itself, known as encephalitis. This is thought to occur in around 1 in 1,000 people who develop viral meningitis from mumps. Encephalitis is a potentially fatal condition that requires admission to a hospital intensive care unit.
About 1 in 20 people with mumps experience some temporary hearing loss, but permanent loss of hearing is rare. It's estimated this occurs in around 1 in 20,000 cases of mumps.
Mumps and pregnancy
In the past it was thought developing mumps during pregnancy increased the risk of miscarriage, but there's little evidence to support this.
However, as a general precaution it's recommended pregnant women avoid close contact with people known to have an active mumps infection (or any other type of infection).
Treatment
Treatment for mumps is focused on relieving symptoms until your body’s immune system fights off the infection. There are currently no medications to treat the mumps virus.
The infection usually passes within a week or two.
In the meantime, the measures below may help.
- get plenty of bed rest until your symptoms have passed
- take over-the-counter painkillers, such as ibuprofen or paracetamol, to relieve any pain (children aged 16 or under should not be given aspirin)
- drink plenty of fluids, but avoid acidic drinks such as fruit juice as these can irritate your parotid glands; water is usually the best fluid to drink
- apply a warm or cool compress to your swollen glands to help reduce any pain
- eat foods that don't require a lot of chewing, such as soup, mashed potatoes and scrambled eggs
If your symptoms don’t improve after seven days, or suddenly worsen, contact your GP for advice.
Please Add your review
Related Questions
Latest published articles
Select a consultation service from the list.
Common Diseases in Nepal
on 15 December, 2021
सेतो दुबी (Vitiligo) सचेतना महिना जुन र बिश्व सेतो दुबी दिवस २०२१
on 21 August, 2021
Kidney Transplantation In Nepal
on 8 August, 2021
COVID-19 Vaccine Centres in Kathmandu
on 1 August, 2021
What is the risk factor for diabetes?
on 10 February, 2021
